Call Us
by Adam Brown
updated July 17, 2020
The rotator cuff is a group of four muscles that attach at the shoulder. They are a small but mighty group that work together to keep the shoulder joint stable and moving efficiently. Tendinopathy affects the part of the muscle that attaches to the bone. These tendons cross through a small space at the top of the shoulder which can make them susceptible to damage from compression or stretching forces causing inflammation, pain and limited movement.
Signs and Symptoms of a Rotator Cuff Problem
Symptoms usually develop gradually and increase over time, but can also result from trauma. You may experience the following:
• deep ache at the side or front of your shoulder
• pain and stiffness with overhead activity or hand behind back motions
• night pain that increases if lying on the affected side
• weakness with rotating or lifting your arm to the side
• protective shoulder hiking
• impaired performance at work or in sport (e.g. swimming, throwing)
Causes of Rotator Cuff Tendonitis
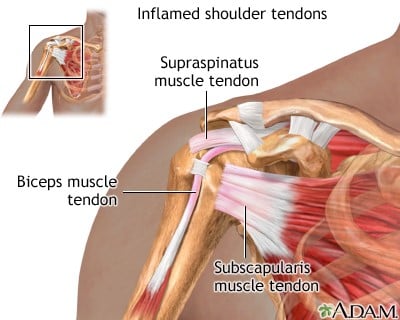
Damage to the rotator cuff can also result from direct trauma to the shoulder or by falling on an outstretched hand.
How Rotator Cuff Tendinitis is Diagnosed
Rotator cuff tendinopathies are best diagnosed through a detailed history and skilled manual testing. Diagnostic tests such as X-ray, MRI, or ultrasound can give you an image of the soft-tissues that are affected, but often don’t correlate well with how well the shoulder is actually functioning.
Physiotherapists can conduct a thorough exam to help find the source of your pain and rule out neck involvement that can often present in the shoulder region. Special tests are used to stress the subacromial space between the arm and shoulder blade to see if your pain is reproduced. These include Hawkins-Kennedy and Neer Impingement tests. Strength is assessed for specific rotator cuff muscle involvement. The ‘empty-can test’ targets the supraspinatus muscle for example.
Treatment for Rotator Cuff Tendonitis
Physiotherapy is the most common and usually most effective treatment for tendinopathies. Physio is aimed at decreasing pain and restoring mobility and function. Exercise to improve posture, rotator cuff endurance and coordination between arm and shoulder blade muscles is often involved. Including mobilization or manipulation of the thoracic spine has been supported in the literature as part of effective treatment for shoulder pathology.
Medications such as NSAIDS are often prescribed to help settle pain, but are not curative. Corticosteroid injections may be recommended if you are not responding to conventional treatment and can provide temporary relief however, frequent injections are not recommended as the can actually cause further damage to the tendons and promote possible tearing.
Surgery is an option for more severe cases and is typically performed arthroscopically through the insertion of a camera and small tools to identify and repair the rotator cuff area. As there are risks associated with surgery, it is usually seen as a last resort.
Prognosis and Outcomes
Most rotator cuff tendinopathies respond extremely well to physiotherapy and you should notice improvement after 6-12 weeks of treatment. However, left untreated there is a likelihood that further gradual damage will occur over time, eventually resulting in partial or complete tearing of the tendon, and changes to the way your shoulder joint moves resulting in early onset of arthritis. Long term, it is important to keep your shoulder muscles strong, and balanced to maintain overall fitness and prevent re-injury.
Final Word
There are many factors involved in most cases of rotator cuff tendonitis and full recovery depends on accurately identifying and correcting all of these causes. Therefore treatment should be specific to each individual patient. If you think you suffer from this condition, please contact one of our nearby physiotherapy clinics to help get better, faster.
Adam Brown MClScPT
Registered Physiotherapist
Adam is a local orthopaedic physiotherapist with extensive experience and training in the treatment of tendonitis impairments. He shares his deep knowledge through regular mentorship of other physiotherapists and healthcare professionals.

Questions? We're happy to help!
Choosing the right service provider can be a big decision. We’re dedicated to answering any questions you have to help you make the best choice. Contact us today and ask us anything!
Call us at (416) 238-6749




