Call Us
What is Osteoarthritis?
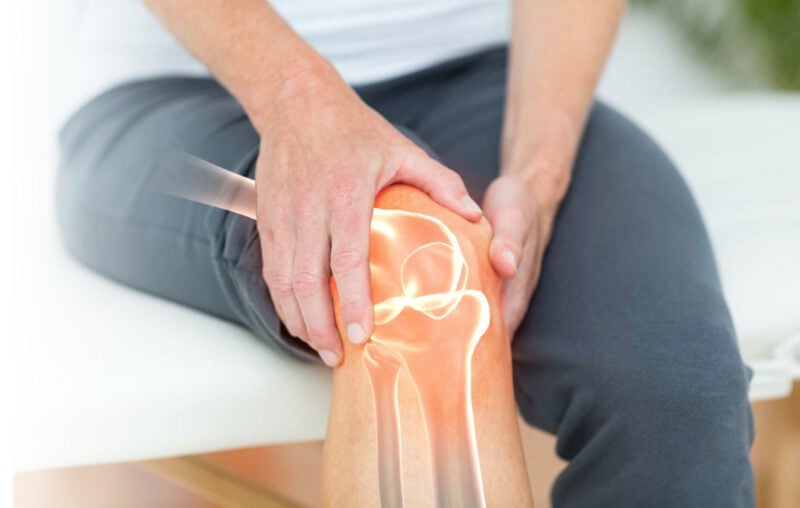
Osteoarthritis is the process of degeneration of cartilage in our joints over time. Cartilage is the protective substance that coats the ends of bones where they come in contact with one another within our joints. Osteoarthritis is often referred to as “wear and tear” arthritis and is commonly referred to simply as “arthritis”. Living with arthritis is a challenge, but it can be managed with a good exercise program.
What are the symptoms of Osteoarthritis?
- Pain: pain is often described as an “ache” and can be present at rest or with movement of the affected joint
- Inflammation: noticeable swelling and warmth to touch may be present around the affected joint
- Joint Stiffness: the affected joint may feel stiff and difficult to move after periods of inactivity (especially first thing in the morning)
- Tenderness: you may find the area around the affected joint is tender or painful to press on
- Reduced Flexibility: the affected joint may lose some range of motion and certain activities like crouching down or getting out of a car become more difficult
- Reduced Strength: you may find some of the things you used to be able to do with the affected joint are more difficult due to reduced strength in the muscles surrounding it
- Crepitus: you may hear pops, clicks, and crackles when moving the affected joint
What joints are affected by Osteoarthritis?
Osteoarthritis most commonly affects the knees and hips but can also affect the joints in our hands and spine.
How is Arthritis diagnosed?
- X-rays: Cartilage loss is revealed by a narrowing of the space between the bones in your joint. As mentioned in one of our previous blog posts, a diagnosis of Osteoarthritis from an X-Ray does not necessarily mean it is the source of your symptoms. Often, X-Rays reveal Osteoarthritis in joints that feel perfectly normal! When Osteoarthritis has progressed to more severe levels, there are a number of treatment options available.
- Magnetic resonance imaging (MRI): An MRI visualizes detailed images of bone and soft tissues including cartilage. An MRI isn’t commonly used to diagnose osteoarthritis but can help provide more information in more complex cases.
- Blood tests: Although there’s no specific blood test for Osteoarthritis, certain markers in your blood can help rule out other inflammatory causes of joint pain such as Rheumatoid Arthritis.
What are the Benefits of Exercise for Osteoarthritis?
Although there are many treatments available for Osteoarthritis, research shows that exercise is the most effective non-pharmacological treatment for reducing pain and improving function in patients. Specifically, exercise improves joint range of motion, muscle flexibility and strength. This helps to improve the body’s ability to move unencumbered and improves overall balance to prevent falls. Exercising can help manage weight, improve mood and protect the aging body from other health conditions.
While you may worry that exercising with Osteoarthritis could harm your joints and cause more pain, the opposite is actually true. When given a personalized exercise program tailored to their specific needs, patients are able to prolong the need for joint replacement surgery and get back to their activities much more quickly.
Exercises For Osteoarthritis
The basic components of an exercise program for Osteoarthritis are activities that improve flexibility, muscle strength, and aerobic endurance.
Exercise should be individually customized to prevent symptom aggravation. Seeing a Physiotherapist at any point in your journey will be beneficial. Whether you are just diagnosed and are looking for strategies to slow the progression, waiting for joint replacement surgery and want to “pre-habilitate”, or you have had joint replacement surgery but have not met your functional goals, Physiotherapy is appropriate. The activities your Physiotherapist prescribes will depend on various factors, including which joints are involved, how severe your pain is, how fit you are, and whether you have other associated medical conditions.
Flexibility (Range of Motion) Exercises for Osteoarthritis
Range of motion refers to the ability to move your joints through the full motion they were designed to achieve. These exercises include dynamic and static gentle stretching. Doing these exercises regularly can help maintain and improve the flexibility of the soft tissues around the affected joints. There is a quote from Physiotherapy school that I will never forget: “Motion is Lotion”. I repeat this to my patients regularly! Home exercises, yoga and Tai Chi are great ways to incorporate flexibility into a daily exercise routine. Improving your joint range of motion will relieve pain and stiffness.
Here are some examples of common range of motion exercises for hips and knees:
Strength (Resistance) Training for Osteoarthritis
These exercises strengthen your muscles to support and protect your joints. Strength training involves contracting the muscles against resistance, whether from your own body or an external resistance source like bands or light weights. Your Physiotherapist will recommend specific exercises based on their assessment of your joints and your symptoms. You should not do strength training more than three to four days per week to allow for adequate rest. If you have joint pain that lasts more than an hour after performing your strengthening exercises, you are probably doing too much.
Here are some examples of common strengthening exercises for hips and knees:
Endurance (Aerobic) Exercise for Osteoarthritis
Low-impact aerobic exercise helps to strengthen the heart and make the lungs work more efficiently. It also reduces fatigue and builds stamina, while helping to control weight. Examples of this type of exercise include walking, jogging, rowing, cycling, climbing stairs, swimming / Aquafit or using the elliptical machine. Canada Health guidelines recommends at least 30 minutes of moderate to vigorous physical activity per day, 3-5 times a week.
Walking
Walking is free and relatively easy on our joints. It also lowers the risk of fractures by stopping or slowing down the loss of bone mass and works muscles that support our joints. If you are worried about your stability with longer distance walks, you can try Nordic pole walking.
Swimming / Aquatic Exercises
Swimming (especially in warm water) can help reduce pain associated with Osteoarthritis, particularly in the large weight bearing joints like hips and knees. The water’s buoyancy helps relieve the pressure of your body’s weight on the affected joints while providing resistance for your muscles to get stronger. Additionally, performing range of motion exercises in shallow or deeper water is helpful for people just beginning to exercise or who have higher pain levels.
What Exercises Should I Avoid with Osteoarthritis?
People with arthritis may need to avoid high impact exercises that put too much pressure or strain on your joints, such as running and sports that involve hopping, quick or sudden turns, or stopping and starting (i.e. tennis, soccer, basketball). A good rule of thumb is that if the activity increases pain during or after exercise, and this persists for several hours (or disturbs your sleep that night), it should be avoided.
If you suspect you have Osteoarthritis or have been diagnosed and are wondering “what’s next”, give Cornerstone Physiotherapy a call to schedule an initial assessment with a Physical therapist. We’d love to help get your health back on track!

Questions? We're happy to help!
Choosing the right service provider can be a big decision. We’re dedicated to answering any questions you have to help you make the best choice. Contact us today and ask us anything!
Call us at (416) 238-6749