BY PHONE
by Rosie Mahendran MScPT
Registered Physiotherapist
updated July 16, 2025
There are many ways we can prepare for the birth of a child, from prepping your home to learning about nutrition – the topics are endless. In this discussion, I want to highlight the best practice to prepare for the labour and delivery of your baby. I understand that sometimes we take the “we’ll just figure it out attitude” (which you will!), but remember knowledge can be powerful.
BEFORE LABOUR AND DELIVERY
1. Choose your health care team, providers and setting.
Should I see an OBGYN or a midwife?
The best answer here is whoever you feel the most comfortable with. Some practical things to know is that both will see you during your pregnancy, during labour and after birth until the 6 week mark. One important consideration might be if you have a specific place you would like to give birth (i.e. OBGYN’s will only deliver in the hospital they are associated with) so if a hospital birth is for you, then they are an option. If you would rather give birth at a birth centre or at home then you are looking at a midwife. Midwives can also deliver in the hospital that they are associated with so are options no matter where you want to birth. They have different training, as midwives are trained in low risk pregnancies while OBGYN’s are both low and high risk. So if you have a condition that puts you in a high risk pregnancy category you need to be with an OBGYN or if you develop something that puts you in this category during pregnancy your care might be transferred to an OBGYN at that time. Another thing some women don’t understand is your OBGYN who follows you through pregnancy may or may not be the one that delivers you as it will depend if they are on call the day/night you go into labour but one of their fellow OBGYN’s at the hospital who is on call will be there for you. Midwives typically work in teams of two so often at least one of the midwives you met during your pregnancy appointments will be at your delivery.
Who should be a part of my birth team?
The research shows that continuous presence of an individual who provides emotional support, comfort measures, advocacy, information and advice during labour helps assist with improved outcomes. These outcomes include, increased likelihood of a vaginal delivery, decreased the use of epidurals, improved APGAR scores and maternal satisfaction. These individuals can include a trained person such as a doula, midwife, nurse and/or friend/family member (SOGC Clinical Practice Guidelines, 2018).
How can pelvic floor physiotherapy help during pregnancy?
Prenatally, pelvic floor physiotherapy is used as a preventative measure and a way to prepare physically and mentally for labour and delivery. This type of therapy can assess the individual and provide information on:
- how to perform Kegels
- how to relax the pelvic floor muscles
- what exercises to partake in
- how to push effectively during labour
- discussion of labour and birthing positions
- how to perform perineal massage
- how to perform mindfulness/breathing strategies during labour/contractions
- what to expect postnatal and how to mitigate some of the common issues women experience
- how to help with low back and pelvic girdle pain, incontinence, pelvic floor heaviness or prolapse, abdominal pain/round ligament pain, pain with transitional movements (turning in bed, rising from sitting etc)
There is strong evidence that pelvic floor muscle training (PFMT) with a physiotherapist is recommended to prevent urinary incontinence during pregnancy and after delivery and core training is recommended to prevent and treat low back and pelvic pain during and following pregnancy (Hay-Smith et al 2008, Joint SOGC/CPA Policy Statement, 2005).
Listen to Episode 65 of the My Fertility Podcast – Why your pelvic floor matters in pregnancy and postpartum, where Cornerstone Pelvic Physiotherapists Courtney Steele and Aparnaa Nandakumar dive into the role of the pelvic floor in pregnancy, delivery, and recovery.
Listen on:
Apple Podcasts
Spotify
Watch on Youtube

Can massage help during pregnancy?
Prenatal massage can help women decrease tension, decrease pain and increase relaxation which promotes overall positive effects for the birthing experience. Prenatal massages can be effective but if you do not have access to massage, gentle touch or pressure from a loved one works as an alternative.
2. Attend a prenatal class.
A prenatal class can cover a wide array of topics and although it is important to attend a prenatal class we also recommend looking into classes that help teach relaxation strategies and educate you about how to prepare YOUR body and mind to prepare the physically and emotionally demanding big life event of giving birth. Traditional prenatal classes cover the essentials of when to call your provider or go to hospital, stages of labour, how to care for baby etc but are not often focused on preparing mom physically for what is to come. Often these classes are great when paired with pelvic floor physiotherapy as it can help increase awareness to the pelvis and reduce potential fear and anxiety around the delivery.
A great starting point for this education/understanding is our FREE VIRTUAL talk we offer once a month on all things pelvic floor as it pertains to pregnancy, birth and postpartum Click here to register for our monthly Belly, Birth & Beyond Class!
3. Make a birth plan!
A general outline of how you want your birth to go can be a great idea. Remember this plan can be modified as you learn more and may not always go accordingly so stay flexible! Your birth plan can include:
- How you want to deliver and where (ex, at a birthing center)
- If you want medical interventions and which ones
- How you want to manage pain
- Who you would like in the delivery room
- How you would like to spend the stages of labour (ex. 1st stage in standing)
4. What types of exercises are safe for me to do during pregnancy?
Exercise is shown to reduce the risk of common complications due to pregnancy. Most exercises have been deemed safe for women according to the Canadian Guidelines for Physical Activity during Pregnancy unless you have contraindications (communicated to you by your healthcare provider). What a better question would be is what exercises are not safe for ME during pregnancy? Exercise prescription no matter what stage of life you are in needs to be individualized and take into account a person’s current physical activity, strength, endurance, likes/dislikes and medical conditions/history. For instance if you were sedentary before your pregnancy taking up crossfit during pregnancy is not a good idea. However, if you were an active crossfitter prior to pregnancy and want to continue this is likely fine with some modifications and assuming no symptoms come on during activities (i.e. pain, incontinence, pelvic heaviness). In general when pregnant women should be cautious about activities that involve physical contact or may involve falling, activities at high altitudes and activities performed in high heat. These activities may include: hockey, horseback riding, gymnastics, hot yoga and skiing. Otherwise, the general recommendations are that pregnant women should:
- Accumulate 150 mins/week of moderate physical activity to reduce complications within pregnancy
- Accumulated over a minimum of 3 days with everyday strongly recommended
- Incorporate aerobic and resistance training exercises and prenatal yoga or gentle stretching
- Pelvic floor muscle training/strengthening (if deemed appropriate by your pelvic floor physiotherapist)
- Maintain adequate nutrition/hydration – drink water before, during and after physical activity
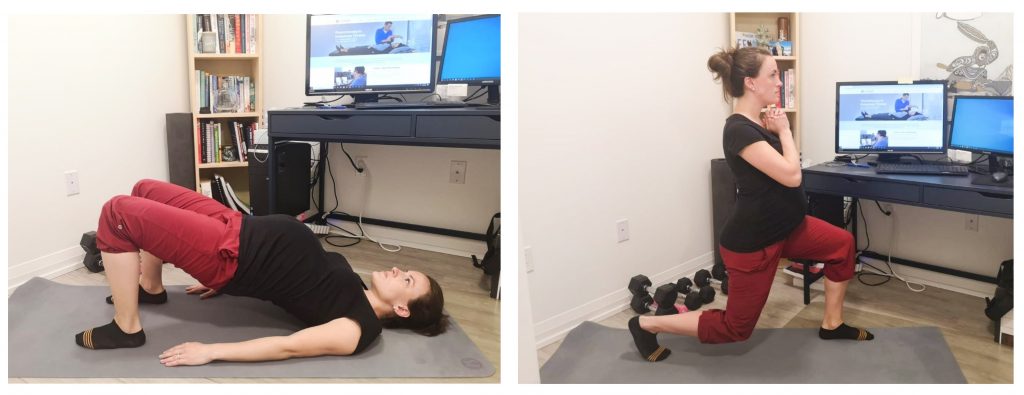
If you were previously inactive you are still encouraged to start physical activity in pregnancy. You may need to begin slower, at a lower intensity and progress gradually. It’s highly recommended you consult a physiotherapist or a fitness professional that works with pregnant individuals to help you progress these activities safely.
DURING LABOUR AND DELIVERY
1. When should I go into the hospital/birthing centre?
In general it is recommended (if possible) to try to spend as much of your labour at home. It is believed that your home can help maintain comfort and as well prevent the use of medical interventions earlier than needed. Typically, you will not be admitted into the hospital until you are 4cm dilated so you can use the 4-1-1 or 5-1-1 rule to estimate what is an appropriate time to go to the hospital or call your midwife. This is when the contractions come every 4 minutes, they last 1 minute in duration and this has been happening for an hour. However, if advised otherwise by your medical professional due to your personal situation or birth history you are to always follow that specific advice.
2. How do I manage my pain?
Many individuals will elect for an epidural to help with any pain experience. If you choose to get an epidural the newest guidelines state that it can be done whenever you need it and based on your choice (SOGC, 2018) . It is important to remember that the epidural requires you to stay still for a certain period of time, so if you are unable to due to pain the anesthesiologist cannot safely administer it.
Other ways that have helped a positive birthing experience and pain include reducing stress. Stress can ramp up your pain experience and also dampen the good hormones we need to facilitate the birthing process. We can reduce stress and pain by:
- creating a calm, environment – this can be achieved by music, low lighting and emotional support
- perform breathing exercises, relaxation/mindfulness techniques, gentle exercises/stretches
- Transcutaneous electrical nerve stimulation (TENS)
- Acupressure/acupuncture
- Heat/cold therapy
- Massage/gentle touch
3. What is the best position to deliver my baby?
In general it is thought that upright, deep squatting or walking can improve the progression of labour and make it easier on a woman’s body to work the baby down in labour. However, some women might find these positions too painful or not available to them.
For the delivery there are also different options here depending on: personal preferences, where you are giving birth, who your care provider is/what they are comfortable with and what is recommended given the specific circumstances at the time and interventions taken or required. Women are often on their backs in hospital if they have had an epidural, however, there may be some options here to improve comfort and ease of delivery. When laying on your back you increase the pressure to the backside of your pelvis/coccyx which we want to have a bit of freedom of movement when the baby is coming. An easy way to do this is to put IV bags or towels under your ischial tuberosities (sit bones) to slightly elevate you so the coccyx is free to move.
A general rule is to assume the most comfortable position for you. You may want to try out these different positions for labouring with your partner ahead of time to see which feels best for you/what you can relax the most in. You should also discuss ahead of time with your health care provider any preferences you may have to see if this is feasible or an option for delivery. Some positions can include:
- 4 point (hands and knees)
- Side lying
- Squatting between partners knees
- Seated on birth chair/stool
- Kneeling
- Knees to chest

4. How do I push?
The same technique does not work for everyone. That being said it is best to practice different options (ideally with guidance and feedback from a pelvic floor physiotherapist) to see what technique you are the best at producing the right amount and length of pressure down to move the baby out effectively. Such techniques can include: low sounds, humming, pursed lip breathing and different imagery cues to help get the pressure directed where we want it. These techniques can relax the muscles and facilitate softening of the muscles to help assist in delivery. As this is not something you have done before, if you are a first time mom it is really helpful to practice and learn ahead of time as you will likely be tired from labour and it is not so easy to learn how to do it at the moment.
AFTER LABOUR AND DELIVERY
1. What do I need to do after birth?
For the first 3 days think about rest, ice, compress and elevation (RICE principles) to help with managing the pain and swelling. Rest (as much as possible under the circumstances) will also help with decreasing your cortisol levels which will improve your healing. We want to avoid excessive force on the healing tissue which may include managing any potential constipation or using some tools to help with easing bowel movements. You can also start gentle pelvic floor muscle training that is pain free – this can help reduce the swelling and feelings of pressure. In this period if you are feeling overwhelmed or have any negative emotions it is important to seek the appropriate care such as maternal support groups, doula, psychologist, etc. Remember you are not alone!
Whether you had a vaginal delivery or cesarean section, at the 6 week mark you should have a check up with your OBGYN/midwife, who will assess the integrity of the tissues. They will deem you safe to return to activities however, they are basing this on tissue healing and not the strength of your pelvic floor, core and rest of your condition to stand up to any and all activities. In France, postnatal women are encouraged to attend 6 pelvic floor physiotherapy sessions (covered by the government) to prevent or treat pelvic floor dysfunctions. Symptoms can present later (after a women starts to become more active) so starting early will help set you on the right track and avoid these symptoms from developing. Postnatally, pelvic floor physiotherapists will assess are:
- Pelvic floor muscles (strength/length/endurance)
- Integrity of C-section scar or vaginal tears
- Your thoughts/beliefs/attitudes and how it affects your physical well-being
- Rectus diastasis (separation of the abdominal musculature)
- Readiness to return to specific activities of interest to you based on the above + overall conditioning
2. When and how can I return to activity or play?
When your physician/midwife has assessed you stitches/scar they will deem you safe to return to activities. You can start with gentle activities (reduced intensity and length) such as yoga, gentle pelvic floor exercises, mommy and me fitness class. You want to monitor for symptoms (such as pressure/heaviness vaginally, incontinence, pain) and if you experience any symptoms scale back the activity or stop. Working with a pelvic floor physiotherapist can be helpful to ease back into activities safely as there are no specific guidelines for exercise for postpartum women.
If you have any questions on how to manage your pregnancy or prepare for childbirth we recommend you set up an appointment with one of our pelvic floor physiotherapists.

Questions? We're happy to help!
Choosing the right service provider can be a big decision. We’re dedicated to answering any questions you have to help you make the best choice. Contact us today and ask us anything!
Call us at (416) 238-6749




